
Intracorneal rings (ICRs) are plastic inserts placed in the cornea. The rings flatten the central cornea to correct low levels of myopia (nearsightedness). Unlike other refractive surgery procedures, ICR procedures can be reversed. When the inserts are removed, the cornea usually returns to its preoperative shape and vision is once again myopic.
The ICR procedure is generally performed on an outpatient basis, using eyedrops for anesthesia. It is a quick procedure and can take less than half an hour.
Research is being done on intracorneal rings for correcting presbyopia (farsightedness) and astigmatism. Rings have recently been used with success in treating corneal disorders such as keratoconus, irregular astigmatism, and progressive corneal thinning that follows other corneal refractive procedures.
Complications with intracorneal rings are rare but can include under-correction, overcorrection, induced astigmatism, infection, glare, halos, and extrusion of the insert. Minimal scarring may also occur in the area of the rings.
The word “laser” is an acronym for Light Amplification by Stimulated Emission of Radiation. A laser is a concentrated beam of light, created when an electrical current passes through a special material. Used in eye surgery since the 1970s, the laser is popular for its unparalleled degree of precision and predictability. Lasers are being used for an increasing variety of eye diseases.
A laser’s specific wavelength allows energy to be absorbed in selected tissues and not damage surrounding tissues. The laser beam is so precise it can cut notches in a strand of human hair without breaking it.
Thermal lasers convert light to heat. This type of laser seals blood vessels and destroys abnormal tissues. Photoablative lasers cut or sculpt tissue and are used to remove tissue, changing the shape and surface of the eye.
For diabetics with diabetic retinopathy, lasers can preserve vision, sometimes for many years. In treating diabetic retinopathy, the laser light seals leaking blood vessels in the retina, the light-sensitive layer of cells lining the back of the eye. Lasers also treat unusual retinal disorders, including blood vessel problems and tumors.
Also used to treat glaucoma, lasers can create a new passage through the iris to relieve eye pressure or open the eye’s blocked drainage canals.
Although lasers do not remove cataracts, they may one day. Right now, they open the posterior capsule, which often becomes cloudy after cataract surgery, restoring vision in a matter of hours.
More recently, the excimer laser has received a great deal of attention as a tool for permanently correcting refractive errors such as nearsightedness, farsightedness, and astigmatism. Refractive laser surgery can decrease or eliminate the need for eyeglasses and contact lenses by reshaping the cornea.
If your cornea is severely damaged or diseased, you might require a corneal transplant to improve your vision.
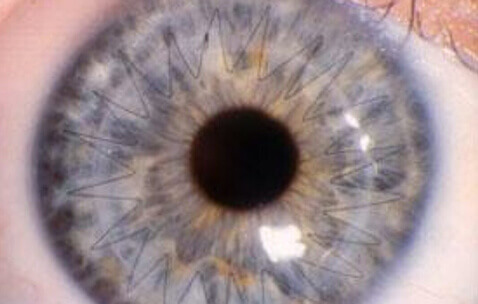
One type of corneal transplant called a penetrating keratoplasty (PKP), replaces your central corneal tissue with donor tissue. The procedure usually takes about an hour under regional or general anesthesia, and you can go home the same day following surgery. After corneal transplant surgery, you will wear a plastic shield or eyeglasses to protect your eye, and you will use eyedrops to prevent infection and rejection of the donor tissue. Your eye doctor will monitor your progress closely after your surgery to ensure the best possible visual outcome and to control minor discomfort associated with the surgery and healing process. Vision usually returns gradually over the next few months or up to a year. It is important to inform your eye doctor if you have pain, irritation, or redness of the eye following PKP, as this could be the earliest sign of infection or rejection, and early treatment of these conditions is critical to the viability of your graft.
Another corneal transplant procedure is called a lamellar keratoplasty. This is an advanced technique that replaces only the superficial layers of your cornea using donor tissue, leaving the lower layers of tissue intact. Although this is a more technically challenging procedure than penetrating keratoplasty, it may reduce the risk that your body will reject the donor tissue and is a good option for some patients.
The newest corneal transplant procedure is called endothelial keratoplasty. This is an advanced technique that replaces the inner layer of your cornea using donor tissue, leaving the upper layers of tissue intact. This treats several conditions such as Fuch’s Dystrophy or other causes of corneal edema (swelling) such as bullous keratopathy. Recovery rates are very good but you must be able to lie flat on your back the first day after surgery in order for the surgery to succeed. Your eye doctor will discuss details of the surgery with you before you have the surgery.