
The cornea is the clear front window of the eye. It covers the iris (the colored portion of the eye) and the round pupil. The cornea is composed of five layers. The outermost layer is called the epithelium.
Injuries to the epithelium, such as scratches, cuts, or scrapes, are known as corneal abrasions . Usually, these injuries are caused by fingernail scratches, makeup brushes, paper cuts, or rubbing of the eyes. Sometimes conditions like dry eye can cause abrasions. Symptoms associated with corneal abrasions include tearing, redness, pain, soreness, and blurred vision.
Treatment options for corneal abrasions include patching the injured eye, dilating pupils to relieve pain, wearing special contact lenses that promote healing, taking antibiotics to prevent infection, and using lubricating eyedrops.
Minor abrasions usually heal within a day or two, while larger abrasions take about a week.
Corneal erosion is caused by a loose attachment of the epithelium to the underlying tissue. This often happens at the site of an earlier abrasion. Some patients have an underlying condition called “map-dot-fingerprint dystrophy” that predisposes them to having recurrent corneal erosions.
Symptoms of corneal erosion are similar to those of abrasions: pain, soreness, redness, and blurred vision.
Treatment is the same as for corneal abrasion and may also include saline solution eyedrops or ointments. However, if the erosion keeps occurring, further treatment may be necessary. These treatments may include procedures to remove the damaged epithelium, removal of corneal cells using a laser, or performing an anterior stromal puncture, which involves making tiny holes on the surface of the cornea to promote stronger attachments between the top layer of corneal cells and the layer of the cornea underneath.
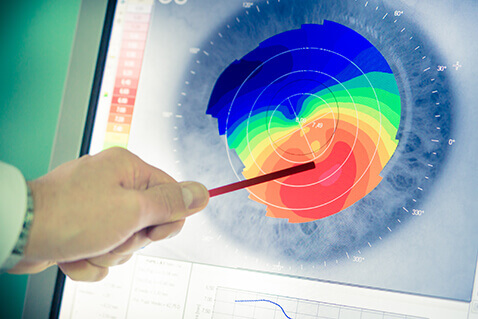
Corneal topography is a computer-assisted procedure used to measure the curvature of the cornea, the clear front window of the eye. The corneal topographer projects illuminated circles on the cornea that are reflected back to the computer and used to produce a map of the cornea. This map can reveal any irregularities in the cornea’s curvature. Other devices measure the corneal elevation in three dimensions, and these measurements are converted into a corneal curvature map.
Corneal topography is commonly used to help follow the progression of keratoconus and to assist in fitting patients with contact lenses to treat the visual distortions caused by this condition. It is also one tool that may be used to help with certain refractive procedures such as LASIK . Following corneal transplant surgery, corneal topography helps the doctor identify where to selectively remove sutures to smooth the shape of the new cornea.
Corneal topography is quick and painless. A technician will ask you to sit comfortably and rest your head against a bar on the topographer. You then look into a lighted bowl. The technician takes a picture, which the computer uses to analyze the curvature of the cornea and to produce an image that the doctor will use in your treatment.
Corneal ulcers, or keratitis, can form due to trauma to the cornea, eyelid disease, severe dry eye, fungus, herpes simplex viral infections, and other causes.
There are two very common types of corneal ulcers. Bacterial ulcers tend to be the most painful type of corneal ulcer, and in some cases, if left untreated, can cause severe damage or even corneal perforation (hole in the eye). Sterile ulcers, on the other hand, usually cause little or no pain.
Improper care and handling of contact lenses, which can lead to infection, are often causes of corneal ulcers.
The symptoms of corneal ulcers may include:
Treatment for corneal ulcers depends on the cause. It usually includes steroid eyedrops, anti-inflammatory drops, or antibiotics. In some cases, hospitalization may be necessary in order to administer eyedrops every hour around the clock, intravenous antibiotics, and other treatments. In rare cases when the cornea is severely damaged, a corneal transplant may be necessary to improve vision.
Ectasia is a condition that occurs when the cornea is so thin that intraocular pressure (IOP) leads to instability and bulging of the cornea. This causes blurring, myopia, and irregular astigmatism.
During laser-assisted in situ keratomileusis (LASIK), the surgeon creates a flap in the outer layer of your cornea and uses the laser to remove some of the lower corneal tissue that is exposed when the flap is moved aside. If your corneas are thinner than normal, you may be at an increased risk for ectasia following LASIK, especially if you require additional LASIK procedures to fine-tune your vision correction. It is even possible (though extremely rare) for ectasia to develop following photorefractive keratectomy (PRK), a surface laser procedure that does not involve creating a corneal flap.
If you have thin corneas, you may not be a good candidate for LASIK. Ask your eye doctor if alternative refractive procedures such as epi-LASIK or PRK might offer you a better chance at improved vision without any unnecessary risk of adverse side effects.
Fuchs’ dystrophy is a progressive disease that affects the cornea, the clear dome that covers the iris (the colored part of the eye) and helps focus light as it enters the eye.
With this disease, cells in the cornea’s inner layer, called the endothelium , are reduced in number. This causes the remaining cells to swell or thicken. The loss of endothelial cells can also allow abnormal dewdrop-shaped growths called guttata to form.
These cell changes may cause the cornea to become cloudy and swollen. Because Fuchs’ dystrophy is a progressive disease, the changes to the cornea can interfere with vision over time. Fuchs’ dystrophy usually occurs in people after age 40. Studies show that it is an inherited condition.
Symptoms of Fuchs’ dystrophy include hazy or cloudy vision that develops in stages. In the first stage, as the cornea swells, vision in the morning may be hazy, but it clears up during the day. Once the disease has progressed to a more advanced stage, vision no longer clears, and instead, you may experience pain and sensitivity to light.
It can take up to 20 years or longer for Fuchs’ dystrophy to progress from its earliest stage to a stage that is visually or physically significant. To diagnose and monitor this condition, an eye doctor checks for adequate endothelial cell number and function, and may measure the thickness of the cornea.
In its early stage, Fuchs’ dystrophy is treated with saline eyedrops to pull excess fluid from the cornea or by using a hairdryer to help dry the surface of the cornea. As Fuchs’ dystrophy advances, you may be given a therapeutic bandage contact lens to lessen your discomfort.
If vision loss begins to interfere with your life in the latter stages of the disease, a partial thickness corneal transplant technique known as endothelial keratoplasty may be performed. This procedure has an excellent success rate.
Fungal keratitis is a serious infection of the cornea-the clear, round dome covering the eye’s iris and pupil. Symptoms of fungal keratitis include:
Risk factors for fungal keratitis include trauma (usually when plant material gets into the eye), chronic or ongoing disease of the surface of the eye, a compromised immune system, and, rarely, contact lens use. Keratitis is not transmitted from person to person.
Fungal keratitis is treated with topical and oral antifungal medications. Patients who do not respond to medical treatment may require eye surgery, possibly including a corneal transplant.
Safe handling, storage, and cleaning of contact lenses are key measures for reducing the risk of infection. You should always use the following safe practices with your lenses:
No matter which cleaning or disinfecting solution you use, consider performing a “rub and rinse” lens cleaning method rather than a “no-rub” method. This can minimize the number of germs on your lenses, reducing your chances of infection.
Herpes keratitis is a viral infection of the eye caused by the herpes simplex virus, best known for causing cold sores. Herpes keratitis usually affects only one eye and most often occurs on the cornea-the normally clear dome that covers the front part of the eye.
The symptoms of herpes keratitis may include:
If the infection is superficial, with ulcers involving only the cornea’s top layer, called the epithelium, it will usually heal without scarring. However, if it involves the deeper layers of the cornea, it may lead to scarring of the cornea, loss of vision, and sometimes even blindness. Left untreated, herpes keratitis can severely damage your eye.
Herpes keratitis is usually treated with antiviral medications, either in eyedrop or pill form. Depending on the progression of the infection, your eye doctor may treat your condition with steroid eyedrops to reduce inflammation. Rarely, when the cornea is severely damaged, a corneal transplant may be necessary to improve vision.
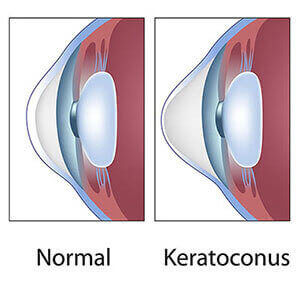
Keratoconus is an uncommon condition in which the dome-shaped cornea (the clear front window of the eye) becomes thin and develops a cone-like bulge. As the condition progresses, the shape of the cornea is altered, distorting your vision. Usually, keratoconus affects both eyes, although symptoms and progression in each eye may differ.
Early symptoms include mild blurring of vision, increased sensitivity to light and glare, and mild eye irritation. The rate of progression varies. Keratoconus usually begins in the teenage years. It may progress slowly for 10 to 20 years and then suddenly stop. As it progresses, the most common symptoms are increased blurring, increased nearsightedness or astigmatism, inability to wear contact lenses, and frequent eyeglass prescription changes.
The causes of keratoconus are not known. Since an estimated 10% of people with keratoconus have a family member with the condition, some researchers believe genetics may play a role.
Keratoconus is usually corrected with eyeglasses. However, as the condition progresses, rigid contact lenses may be needed so that vision is improved. If vision is greatly affected, a corneal transplant may be recommended. While this procedure will relieve the symptoms of keratoconus, it will not cure it completely. Nonetheless, corneal transplants offer the best prognosis for clear vision.
A new technique recently has been evaluated to treat progressive keratoconus. This technique involves placing crescent-shaped acrylic inserts in the midperiphery of the cornea. This has been shown to be effective in some patients. You should discuss this technology with your eye doctor.
Lid margin disease is a common and frequently chronic inflammation of the eyelids. Symptoms include irritation, itching, and, occasionally, a red eye. This condition frequently occurs in people who tend to have oily skin, dandruff, or dry eyes.
Bacteria normally reside on the skin, but in some people, they thrive in the skin at the base of the eyelashes. Nearby oil glands may be overactive, causing dandruff-like scales and particles to form along the lashes and eyelid margins, which can cause redness, stinging, or burning.
Lid margin disease cannot be cured, but it can be controlled with a few simple, daily hygienic measures, such as the following:
When medications are necessary, they may include:
Medications alone are not sufficient to control lid margin disease; the application of warmth and detailed cleansing of the lashes daily is the key.
A pterygium is a mass of fleshy tissue that grows over the cornea (the clear front window of the eye). It may remain small or may grow large enough to interfere with vision. A pterygium most commonly occurs on the inner corner of the eye, but it can appear on the outer corner as well.
The exact cause of pterygia is not well understood. They occur more often in people who spend a lot of time outdoors, especially in sunny climates. Long-term exposure to sunlight, especially to ultraviolet (UV) rays, and chronic eye irritation from dry, dusty conditions seem to play an important role. Dry eye also may contribute to pterygium.
When a pterygium becomes red and irritated, eyedrops or ointments can be used to help reduce the inflammation. If the pterygium grows rapidly or is large enough to threaten sight, it can be removed surgically.
Despite proper surgical removal, a pterygium may return, particularly in young people. Protecting the eyes from excessive ultraviolet light with proper sunglasses, avoiding dry, dusty conditions, and using artificial tears can also help.
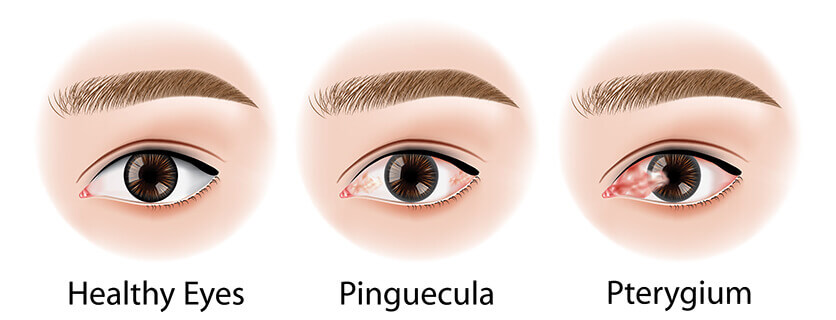
A pinguecula is a yellowish patch or bump on the white of the eye, most often on the side closest to the nose. It is not a tumor but is an alteration of normal tissue resulting in a deposit of protein and fat. Unlike a pterygium, a pinguecula does not actually grow onto the cornea. A pinguecula can also be a response to chronic eye irritation or sunlight.
No treatment is necessary unless the pinguecula becomes inflamed. A pinguecula does not grow onto the cornea or threaten sight. On rare occasions, a pinguecula can be surgically removed if it is particularly annoying.
The cornea is the clear front window of the eye. It covers the iris (the colored portion of the eye) and the round pupil. The cornea is composed of five layers. The outermost layer is the epithelium.
When the epithelium does not adhere correctly to the corneal tissue below, this can cause a condition called recurrent corneal erosion .
There are many possible causes of recurrent corneal erosion, including a history of corneal injury, such as corneal abrasion, and corneal disease.
Symptoms include:
Often symptoms are first noticed upon waking in the morning. This is because when you open your eyes, your eyelids pull away the cells that have been loosened overnight. Without treatment, your eye may continue to experience this erosion.
To detect and evaluate corneal erosion, your eye doctor will instill eyedrops with green or yellow dye in your eye and examine your eyes using a slit-lamp microscope. Your eye doctor may prescribe saline solution drops to help your epithelium adhere to the underlying tissue, and he or she also may ask you to use artificial tears to keep your eyes moist.
For patients with corneal erosion caused by corneal disease, an additional procedure may be necessary to remove the epithelium or adhere it to the underlying tissue in order to encourage a better bond.
Should you continue to experience recurrent corneal erosion despite conservative treatments, your eye doctor might suggest an additional procedure called a phototherapeutic keratectomy to remove a layer of corneal tissue with a laser. This technique is used to promote healing and good adherence of the epithelium.