Because it has no noticeable symptoms, glaucoma is a difficult disease to detect without regular, complete eye exams.
During a glaucoma evaluation, your eye doctor will perform the following tests:
Tonometry: The pressure in your eyes (intraocular pressure, or IOP) is measured using a technique called tonometry. Tonometry measures your IOP by determining how your cornea responds when an instrument (or sometimes a puff of air) presses on the surface of your eye. Eye drops are used to numb the surface of your eye for this test.
Gonioscopy: For this test, your eye doctor inspects your eye’s drainage angle-the area where fluid drains out of your eye. During gonioscopy, you sit in a chair facing the microscope used to look inside your eye. You will place your chin on a chin rest and your forehead against a support bar while looking straight ahead. The goniolens is placed lightly on the front of your eye, and a narrow beam of light is directed into your eye while your doctor looks through the slit lamp at the drainage angle. Drops will be used to numb the eye before the test.
Ophthalmoscopy: With this test, your eye doctor can evaluate whether or not there is any optic nerve damage by looking at the back of the eye (called the fundus). There are two types of ophthalmoscopy: direct and indirect. With direct ophthalmoscopy, your ophthalmologist uses a small flashlight-like instrument with several lenses that magnifies up to about 15 times. This type of ophthalmoscopy is most commonly done during a routine physical examination. With indirect ophthalmoscopy, the ophthalmologist wears a headband with a light attached and uses a small handheld lens to look inside your eye. Indirect ophthalmoscopy allows a better view of the fundus, even if your natural lens is clouded by cataracts.
Visual Field Test: The peripheral (side) vision of each eye is tested with visual field testing, or perimetry. For this test, you sit at a bowl-shaped instrument called a perimeter. While you stare at the center of the bowl, lights will flash off and on. Each time you see a flash, you press a button. A computer records your response to each flash. This test shows if you have any areas of loss of side vision. Loss of peripheral vision is often an early sign of glaucoma.
Photography: Sometimes photographs or other computerized images are taken of the optic nerve to inspect the nerve more closely for damage from elevated pressure in the eye.
Special Imaging: Different scanners may be used to better determine the configuration of the optic nerve head or retinal nerve fiber layer.
Each of these evaluation tools is an important way to monitor your vision to help ensure that glaucoma does not rob you of your sight. Some of these tests will not be necessary for everyone. Your ophthalmologist will discuss which tests are best for you. Some tests may need to be repeated on a regular basis to monitor any changes in your vision caused by glaucoma.
Glaucoma is a disease of the optic nerve, which transmits the images you see from the eye to the brain. The optic nerve is made up of many nerve fibers (like an electric cable with its numerous wires). Glaucoma damages nerve fibers, which can cause blind spots and vision loss.
Glaucoma has to do with the pressure inside the eye, known as intraocular pressure (IOP). When the aqueous humor (a clear liquid that normally flows in and out of the eye) cannot drain properly, pressure builds up in the eye. The resulting increase in IOP can damage the optic nerve and lead to vision loss.
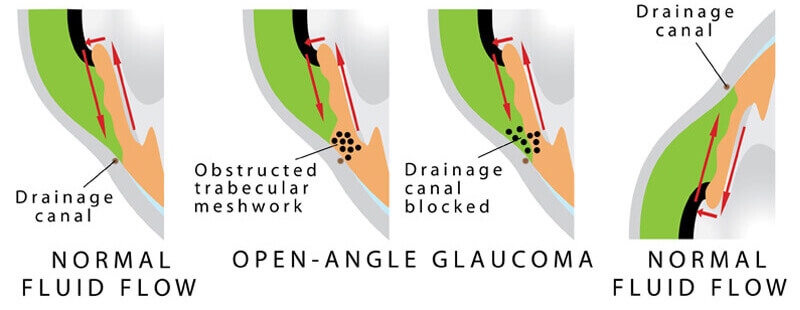
The most common form of glaucoma is primary open-angle glaucoma, in which the aqueous fluid is blocked from flowing back out of the eye at a normal rate through a tiny drainage system. Most people who develop primary open-angle glaucoma notice no symptoms until their vision is impaired.
Ocular hypertension is often a forerunner to actual open-angle glaucoma. When intraocular pressure is above normal, the risk of developing glaucoma increases. Several risk factors will affect whether you will develop glaucoma, including the level of IOP, family history, and the corneal thickness. If your risk is high, your eye doctor may recommend treatment to lower your IOP to prevent future damage.
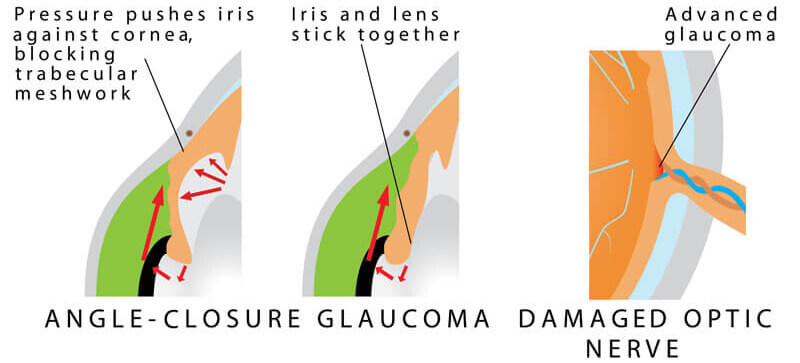
In angle-closure glaucoma, the iris (the colored part of the eye) may drop over and completely close off the drainage angle, abruptly blocking the flow of aqueous fluid and leading to increased IOP and optic nerve damage. In acute angle-closure glaucoma, there is a sudden increase in IOP due to the buildup of aqueous fluid. This condition is considered an emergency because optic nerve damage and vision loss can occur within hours of the problem. Symptoms can include nausea, vomiting, seeing halos around lights, and eye pain.
Even some people with “normal” IOP can experience vision loss from glaucoma. This condition is called normal-tension glaucoma. In this type of glaucoma, the optic nerve is damaged even though the IOP is considered normal. Normal-tension glaucoma is not well understood, but lowering IOP has been shown to slow the progression of this form of glaucoma.
Childhood glaucoma, which starts in infancy, childhood, or adolescence, is rare. Like primary open-angle glaucoma, there are few, if any, symptoms in the early stage. Blindness can result if it is left untreated. Like most types of glaucoma, childhood glaucoma may run in families. Signs of this disease include:
Your eye doctor may tell you that you are at risk for glaucoma if you have one or more risk factors, including having an elevated IOP, a family history of glaucoma, certain optic nerve conditions, are of a particular ethnic background, or are of advanced age. Regular examinations with your eye doctor are important if you are at risk for this condition.
The goal of glaucoma treatment is to lower your eye pressure to prevent or slow further vision loss. Your doctor will recommend treatment if the risk of vision loss is high. Treatment often consists of eye drops but can include laser treatment or surgery to create a new drain in the eye. Glaucoma is a chronic disease that can be controlled but not cured. Ongoing monitoring (every three to six months) is needed to watch for changes. Ask your eye doctor if you have any questions about glaucoma or your treatment.
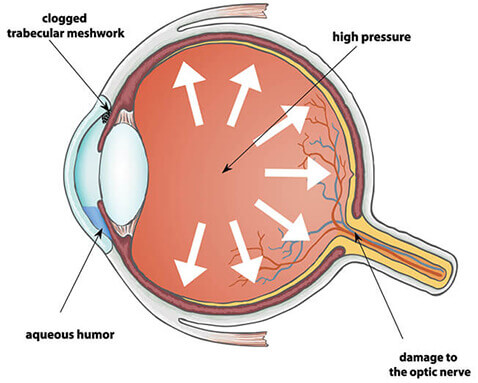
Elevated intraocular pressure (high pressure within the eye) is the number one risk factor for glaucoma. However, elevated intraocular pressure (IOP) does not always cause glaucoma.
The average eye pressure in adults ranges between 10 mm Hg and 21 mm Hg (“mm Hg” stands for “millimeters of mercury”). There can be a significant difference in your IOP throughout the course of a day. This variation is known as diurnal fluctuation. We know that many patients with IOP in the 20s do not develop glaucoma. Up to 50% of patients diagnosed with glaucoma have an initial pressure reading lower than 22 mm Hg. Intraocular pressure is not a very sensitive tool for diagnosing glaucoma, but it becomes very useful in monitoring treatment for glaucoma.
A variety of methods can be used to check the intraocular pressure, but the most common are applanation tonometry and pneumotonometry. Your eye doctor will often set a “target” pressure for you and will adjust the treatment to keep the pressure close to or below that target to help preserve your vision.
Early in the disease process of glaucoma, individual nerve fibers in the eye’s optic nerve are lost, causing an associated pattern of nerve-fiber-layer thinning. This problem can later translate into loss of tissue at the optic nerve head, resulting in visual field defects and, ultimately, loss of vision.
New techniques have been devised to help measure the thickness of the nerve fiber layer, helping eye doctors diagnose glaucoma earlier and monitor progression of the disease.
One technique used to measure the nerve fiber layer is called scanning laser polarimetry, which utilizes a device called a GDx scanner. Another technique uses a low-power laser light and a process called optical coherence tomography (OCT). These new imaging techniques can help provide an objective measurement of the nerve fiber layer, enhancing the ability to effectively diagnose and monitor glaucoma.
Both tests are done in the doctor’s office. During these tests, the patient is required only to remain still while the image is scanned.
Pigmentary dispersion syndrome is a condition in which increased amounts of pigment circulate within the front portion of the eye. This often results in having pigment layered on the back of the cornea, thinning of the iris, and clogging of the ocular drainage system with pigment. This pigment can block the drainage channel enough to cause an increase in intraocular pressure (IOP).
In cases of pigmentary glaucoma, the IOP often is very high, reaching levels above 40. Pigmentary dispersion leads to damage from glaucoma in 20% to 50% of patients. It is more common in males and often appears in people under 50 years of age.
Treatment is the same as for other forms of open-angle glaucoma, including medications, laser therapy, or surgery. With adequate treatment, the prognosis for pigmentary glaucoma is good.
Pseudoexfoliation glaucoma is a relatively common form of open-angle glaucoma that can cause significantly high eye pressures. This condition is marked by a dust-like material that is observed inside the eye on the surface of the iris and lens. This material can clog the ocular drainage system, increasing intraocular pressure (IOP). It can occur in one or both eyes and is most commonly seen in patients over the age of 70. Pseudoexfoliation glaucoma is found in all ethnic groups, but it is most commonly seen in people of Scandinavian ancestry.
Treatment is often required for pseudoexfoliation glaucoma, consisting of medication, laser treatment, or surgery. Pseudoexfoliation can cause increased complications with cataract surgery. With proper treatment and monitoring, patients with pseudoexfoliation glaucoma tend to do well. Early diagnosis is important.
If your eye is injured, there is a chance you will develop traumatic glaucoma. A direct blow to the eye can cause bleeding or inflammation in the eye, which may lead to an acute rise in eye pressure. This condition can typically be managed with eye drop medication. However, if the intraocular pressure (IOP) is very high or if blood remains in the eye, surgical treatment may be required.
If an eye is hit hard enough to cause bleeding in the front part of the eye, this is called a hyphema. A hyphema increases the possibility of a rise in eye pressure. Various medications can bring the pressure down to a safe zone until the blood decreases or disappears.
In cases of a hyphema, there is also a chance of a future increase in eye pressure. The chance of developing elevated eye pressure and glaucoma following a hyphema is thought to be approximately 8% over a patient’s lifetime. Therefore, anyone who has had eye trauma should be sure to have intraocular pressure checks every year. If your eye doctor notes an increase in your eye pressure, he or she can find ways to control it.
Because it has no noticeable symptoms, glaucoma is a difficult disease to detect without regular, complete eye exams.
One particular test called a visual field test (also called perimetry ), measures all areas of your eyesight, including your side, or peripheral, vision. A visual field test can help find certain patterns of vision loss and is a key way to check for glaucoma. It is very useful in finding early changes in vision caused by nerve damage from glaucoma.
To take this painless test, you sit at a bowl-shaped instrument called a perimeter. While you stare at the center of the bowl, lights flash. Each time you see a flash you press a button. A computer records the location of each flash and whether you pressed the button when the light flashed in that location. At the end of the test, a printout shows if there are areas of your field of vision where you did not see the flashes of light. This test shows if you have any areas of vision loss. Loss of peripheral vision (also known as side vision ) is often an early sign of glaucoma. Regular perimetry tests are an important technique for learning how, if at all, your vision is changing over time. It can also be used to see if treatment for glaucoma is preventing further vision loss.